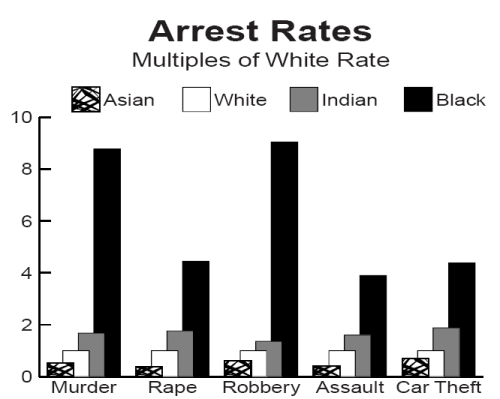
After a long argument with a vegan, I decided to track down all the studies on bone density and protein I could, to find out just what the evidence was for vegetarian claims that animal protein causes problems with bone mass. Out of all these studies, the last four agree with the veggie point of view (in red), all the others show no effect or positive effects from animal protein. (blue). There were three overviews, of which two were actual meta studies, which I placed at the end as they are pretty much definitive (and are slightly pro protein). Pro animal protein totals 17, neutral 2, anti 4. Which makes 19 v 4. Pro animal protein wins, I guess. Although one was anvague overview, and one was of a pretty restrictive diet, which takes it to 18 v 3. Funny how it’s only the handful that show a loss that make it onto the veggie sites.
In all things, a sense of proportion is crucial.
The Effects of Dietary Protein on Bone Mineral Mass in Young Adults May Be Modulated by Adolescent Calcium Intake1,2
The effect of dietary protein on bone mass measures at different life stages is controversial. We investigated the influence of protein intake on bone mass measures in young adults, considering the influence of calcium intake through adolescence. Subjects were 133 young adults (59 males, 74 females) who were participating in the Saskatchewan Pediatric Bone Mineral Accrual Study (1991–1997, 2003–2006). At adulthood, their mean age was 23 y. We assessed dietary intake via serial 24-h recalls carried out at least once yearly. Total body (TB) bone mineral content (BMC) and TB bone mineral density (BMD) were assessed annually using Dual energy X-ray absorptiometry. We determined TB-BMC net gain from the age of peak height velocity (PHV) to early adulthood. We analyzed data from all subjects and subsets based on sex and calcium intake using multiple regression. TB-BMC significantly increased from age at PHV to early adulthood by 41% in males and 37% in females. Height, weight, physical activity, and sex were significant predictors of TB-BMC, TB-BMC net gain, and TB-BMD among all subjects. Protein intake predicted TB-BMC net gain in all subjects (ß = 0.11; P = 0.015). In females at peri-adolescence or early adulthood with adequate calcium intake (>1000 mg/d), protein intake positively predicted TB-BMC, TB-BMC net gain, and TB-BMD (P < 0.05). Our results indicate that when calcium intake is adequate, protein intake has a beneficial effect on the bone mass of young adult females. Protein, in the absence of sufficient calcium, does not confer as much benefit to bone.
Dietary protein intakes and bone growth
Peak bone mass is a significant determinant of fracture risk later in life. Nutritional intakes, particularly proteins, are able to modulate the genetic potential, with effects starting as early as in utero. There is a positive correlation between yearly lumbar and femoral bone mass gain, and protein intake. Dairy products consumption positively influences bone mineral density at the spine, hip and forearm in adolescents, leading thereby to a higher peak bone mass. Nutritional intakes, particularly proteins, are associated to bone growth, hence to bone strength and resistance to fracture later in life. The growth hormone IGF-I-target organ axis is likely to be implicated in this process. Variations in the protein intake within the “normal” range can have a significant effect on skeletal growth and thereby modulate the genetic potential in peak bone mass attainment.
Dietary Protein: An Essential Nutrient For Bone Health
Nutrition plays a major role in the development and maintenance of bone structures resistant to usual mechanical loadings. In addition to calcium in the presence of an adequate vitamin D supply, proteins represent a key nutrient for bone health, and thereby in the prevention of osteoporosis. In sharp opposition to experimental and clinical evidence, it has been alleged that proteins, particularly those from animal sources, might be deleterious for bone health by inducing chronic metabolic acidosis which in turn would be responsible for increased calciuria and accelerated mineral dissolution. This claim is based on an hypothesis that artificially assembles various notions, including in vitro observations on the physical-chemical property of apatite crystal, short term human studies on the calciuric response to increased protein intakes, as well as retrospective inter-ethnic comparisons on the prevalence of hip fractures. The main purpose of this review is to analyze the evidence that refutes a relation of causality between the elements of this putative patho-physiological “cascade” that purports that animal proteins are causally associated with an increased incidence of osteoporotic fractures. In contrast, many experimental and clinical published data concur to indicate that low protein intake negatively affects bone health. Thus, selective deficiency in dietary proteins causes marked deterioration in bone mass, micro architecture and strength, the hallmark of osteoporosis. In the elderly, low protein intakes are often observed in patients with hip fracture. In these patients intervention study after orthopedic management demonstrates that protein supplementation as given in the form of casein, attenuates post-fracture bone loss, increases muscles strength, reduces medical complications and hospital stay. In agreement with both experimental and clinical intervention studies, large prospective epidemiologic observations indicate that relatively high protein intakes, including those from animal sources are associated with increased bone mineral mass and reduced incidence of osteoporotic fractures. As to the increased calciuria that can be observed in response to an augmentation in either animal or vegetal proteins it can be explained by a stimulation of the intestinal calcium absorption. Dietary proteins also enhance IGF-1, a factor that exerts positive activity on skeletal development and bone formation. Consequently, dietary proteins are as essential as calcium and vitamin D for bone health and osteoporosis prevention. Furthermore, there is no consistent evidence for superiority of vegetal over animal proteins on calcium metabolism, bone loss prevention and risk reduction of fragility fractures.
Elderly Women Need Dietary Protein to Maintain Bone Mass
Excess dietary protein is considered a risk factor for osteoporosis owing to the potential for renal acid load. Researchers who conducted a recent prospective study of older adults reported that animal protein had a protective role for bone, especially in elderly women, whereas plant protein was negatively associated with bone mineral density. An interaction between protein and calcium suggested protein alone was not the important factor. Other studies confirm the beneficial effect of increasing dietary protein intake in older women to reduce bone mineral density loss and risk of fracture, suggesting that emphasis should be placed on promoting adequate protein intake in elderly women.
Animal protein and bone growth – Scientific substantiation of a health claim related to animal protein and bone growth pursuant to Article 14 of Regulation (EC) No 1924/2006[1] – Scientific Opinion of the Panel on Dietetic Products, Nutrition and Allergies
The evidence provided by consensus opinions/reports from authoritative bodies and reviews shows that there is good consensus on the role of protein in growth and development of bone. It is well established that a source of protein is essential for allowing both growth and maintenance.
Interaction of Dietary Calcium and Protein in Bone Health in Humans1,2
Protein has both positive and negative effects on calcium balance, and the net effect of dietary protein on bone mass and fracture risk may be dependent on the dietary calcium intake. In addition to providing substrate for bone matrix, dietary protein stimulates the production of insulin-like growth factor-1 (IGF-1), a factor that promotes osteoblast-mediated bone formation. Protein also increases urinary calcium losses, by several proposed mechanisms. Increasing calcium intake may offset the negative impact of dietary protein on urinary calcium losses, allowing the favorable effect of protein on the IGF-1 axis to dominate. Several, although not all, studies are either compatible with or support this hypothesis. Protein supplements significantly reduced bone loss in elderly hip-fracture patients in a study in which both the protein and control groups received supplemental calcium. In an observational study, total protein intake was positively associated with favorable 3-y changes in femoral neck and total body bone mineral density in volunteers who received supplemental calcium citrate malate and vitamin D, but not in volunteers taking placebos. In conclusion, an adequate calcium intake may help promote a favorable effect of dietary protein on the skeleton in older individuals.
Milk basic protein increases bone mineral density and improves bone metabolism in healthy young women.
Effect of milk basic protein on bone metabolism in healthy young women.
INTRODUCTION: Milk has more beneficial effects on bone health than other food sources. Recent in vitro and in vivo studies have shown that milk whey protein, especially its basic protein fraction (milk basic protein, MBP), contains several components capable of promoting bone formation and inhibiting bone resorption. The object of this study was to examine the effect of MBP on the bone mineral density and bone metabolism of healthy young women.METHODS: Thirty-five healthy young women were randomly assigned to treatment with either placebo or MBP (40 mg per day) for 6 months. The bone mineral density (BMD) of the lumbar vertebrae L2-L4 of each subject was measured by dual-energy X-ray absorptiometry (DXA) at 0 and 6 months of treatment. Serum and urine indexes of bone metabolism were measured at 0, 3 and 6 months. All subjects completed the study in accordance with the protocol.RESULTS: The mean rate of gain of lumbar BMD in the MBP group (1.57%) was significantly higher than in the placebo group (0.13%, P=0.042). When compared with the placebo group, urinary cross-linked N-telopeptides of type-I collagen (NTx) were significantly decreased, and serum osteocalcin was significantly increased in the MBP group at 6 months.CONCLUSION: These results suggested that MBP supplementation was effective in increasing BMD in young women and that this increase in BMD may be primarily mediated through the promotion of bone formation and inhibition of bone resorption by MBP supplementation.
Dietary Protein: An Essential Nutrient For Bone Health
Nutrition plays a major role in the development and maintenance of bone structures resistant to usual mechanical loadings. In addition to calcium in the presence of an adequate vitamin D supply, proteins represent a key nutrient for bone health, and thereby in the prevention of osteoporosis. In sharp opposition to experimental and clinical evidence, it has been alleged that proteins, particularly those from animal sources, might be deleterious for bone health by inducing chronic metabolic acidosis which in turn would be responsible for increased calciuria and accelerated mineral dissolution. This claim is based on an hypothesis that artificially assembles various notions, including in vitro observations on the physical-chemical property of apatite crystal, short term human studies on the calciuric response to increased protein intakes, as well as retrospective inter-ethnic comparisons on the prevalence of hip fractures. The main purpose of this review is to analyze the evidence that refutes a relation of causality between the elements of this putative patho-physiological “cascade” that purports that animal proteins are causally associated with an increased incidence of osteoporotic fractures. In contrast, many experimental and clinical published data concur to indicate that low protein intake negatively affects bone health. Thus, selective deficiency in dietary proteins causes marked deterioration in bone mass, micro architecture and strength, the hallmark of osteoporosis. In the elderly, low protein intakes are often observed in patients with hip fracture. In these patients intervention study after orthopedic management demonstrates that protein supplementation as given in the form of casein, attenuates post-fracture bone loss, increases muscles strength, reduces medical complications and hospital stay. In agreement with both experimental and clinical intervention studies, large prospective epidemiologic observations indicate that relatively high protein intakes, including those from animal sources are associated with increased bone mineral mass and reduced incidence of osteoporotic fractures. As to the increased calciuria that can be observed in response to an augmentation in either animal or vegetal proteins it can be explained by a stimulation of the intestinal calcium absorption. Dietary proteins also enhance IGF-1, a factor that exerts positive activity on skeletal development and bone formation. Consequently, dietary proteins are as essential as calcium and vitamin D for bone health and osteoporosis prevention. Furthermore, there is no consistent evidence for superiority of vegetal over animal proteins on calcium metabolism, bone loss prevention and risk reduction of fragility fractures.
Dietary whey protein concentrate partially alleviates the decrease in bone density observed with high protein diet
Protein intake: effects on bone mineral density and the rate of bone loss in elderly women1,2,3,4
Results: In the cross-sectional study, a higher intake of protein was associated with higher BMD. BMD was significantly higher (P < 0.05) in the spine (7%), midradius (6%), and total body (5%) in subjects in the highest quartile of protein intake than in those in the lower 2 quartiles. This positive association was seen in women with calcium intakes > 408 mg/d. There was no significant effect of protein intake on hip BMD. In the longitudinal study of the placebo group, there was no association between protein intake and the rate of bone loss.
Conclusions: The highest quartile of protein intake (: 72 g/d) was associated with higher BMD in elderly women at baseline only when the calcium intake exceeded 408 mg/d. In the longitudinal study, no association was seen between protein intake and the rate of bone loss, perhaps because the sample size was too small or the follow-up period of 3 y was not long enough to detect change
A positive association of lumbar spine bone mineral density with dietary protein is suppressed by a negative association with protein sulfur.
Dietary protein is theorized to hold both anabolic effects on bone and demineralizing effects mediated by the diet acid load of sulfate derived from methionine and cysteine. The relative importance of these effects is unknown but relevant to osteoporosis prevention. Postmenopausal women (n=161, 67.9±6.0 y) were assessed for areal bone mineral density (aBMD) of lumbar spine (LS) and total hip (TH) using dual X-ray absorptiometry, and dietary intakes of protein, sulfur-containing amino acids, and minerals using a USDA multiple-pass 24-h recall. The acidifying influence of the diet was estimated using the ratio of protein:potassium intake, the potential renal acid load (PRAL), and intake of sulfate equivalents from protein. aBMD was regressed onto protein intake then protein was controlled for estimated dietary acid load. A step-down procedure assessed potential confounding influences (weight, age, physical activity, and calcium and vitamin D intakes). Protein alone did not predict LS aBMD (P=0.81); however, after accounting for a negative effect of sulfate (β=-0.28; P<0.01), the direct effect of protein intake was positive (β=0.22; P=0.04). At the TH, protein intake predicted aBMD (β=0.18; P=0.03), but R2 did not improve with adjustment for sulfate (P=0.83). PRAL and the protein:potassium ratio were not significant predictors of aBMD. Results suggest that protein intake is positively associated with aBMD, but benefit at the LS is offset by a negative impact of the protein sulfur acid load. If validated experimentally, these findings harmonize conflicting theories on the role of dietary protein in bone health.
PROTEIN INTAKE AND SITE SPECIFIC BONE MINERAL DENSITY IN CAUCASIAN MALE RESISTANCE TRAINERS
As hypothesized, this research showed that there was no significant difference between protein-seeking resistance trainers and non-protein seeking resistance trainers in relation to site-specific BMD. This research also displayed that site-specific BMD can produce different results than seen with the whole body BMD.
Low Protein Intake: The Impact on Calcium and Bone Homeostasis in Humans1,2
There is agreement that diets moderate in protein (in the approximate range of 1.0 to 1.5 g protein/kg) are associated with normal calcium metabolism and presumably do not alter skeletal homeostasis. Approximately 30–50% of adults in the United States consume dietary protein that could be considered moderate. At low protein intakes, intestinal calcium absorption is reduced, resulting in increases in serum PTH and calcitriol that persist for at least 2–4 wk. The long-term implications of these findings are unknown; however, recent epidemiological data suggest increased rates of bone loss in individuals consuming such diets. Individuals consuming high protein intakes, particularly from omnivorous sources, develop hypercalciuria that is attributable for the most part to an increase in intestinal calcium absorption. Whether high protein diets result in an increase in bone resorption and higher fracture rates remains uncertain.
Does dietary protein reduce hip fracture risk in elders? The Framingham Osteoporosis Study.
RESULTS: Among 946 participants (mean age 75 years), mean protein intake was found to be 68 gm/d. Increased protein intake was associated with a decreased risk of hip fracture compared to those in the lowest quartile of protein intake (Q2 HR = 0.70, Q3 HR = 0.56, and Q4 HR = 0.63; all p values ≥ 0.044), p for trend was 0.07. When a threshold effect was considered (Q2-4 vs Q1), intakes in the higher quartiles combined were associated with a significantly lower risk for hip fracture (HR = 0.63; p = 0.04).
CONCLUSION: Our results are consistent with reduced risk of hip fracture with higher dietary protein intake. Larger prospective studies are needed to confirm and extend this finding in elderly men and women.
Prospective study of dietary protein intake and risk of hip fracture in postmenopausal women1,2,3
Results: Forty-four cases of incident hip fractures were included in the analyses of 104338 person-years (the number of subjects studied times the number of years of follow-up) of follow-up data. The risk of hip fracture was not related to intake of calcium or vitamin D, but was negatively associated with total protein intake. Animal rather than vegetable sources of protein appeared to account for this association. In a multivariate model with inclusion of age, body size, parity, smoking, alcohol intake, estrogen use, and physical activity, the relative risks of hip fracture decreased across increasing quartiles of intake of animal protein as follows: 1.00 (reference), 0.59 (95% CI: 0.26, 1.34), 0.63 (0.28, 1.42), and 0.31 (0.10, 0.93); P for trend = 0.037. Conclusion: Intake of dietary protein, especially from animal sources, may be associated with a reduced incidence of hip fractures in postmenopausal women
Dietary Protein Intake and Risk of Osteoporotic Hip Fracture in Elderly Residents of Utah†
The role of protein intake in osteoporosis is unclear. In a case-control study in Utah (n = 2501), increasing level of protein intake was associated with a decreased risk of hip fracture in men and women 50–69 years of age but not in those 70–89 years of age. Protein intake may be important for optimal bone health.
Results: In logistic regression analyses that controlled for gender, body mass index, smoking status, alcohol use, calcium, vitamin D, potassium, physical activity, and estrogen use in women, the odds ratios (OR) of hip fracture decreased across increasing quartiles of total protein intake for participants 50–69 years of age (OR: 1.0 [reference]; 0.51 [95% CI: 0.30–0.87]; 0.53 [0.31–0.89]; 0.35 [0.21–0.59]; p < 0.001). No similar associations were observed among participants 70–89 years of age. Results from analyses stratified by low and high calcium and potassium intake did not differ appreciably from the results presented above.
Conclusion: Higher total protein intake was associated with a reduced risk of hip fracture in men and women 50–69 years of age but not in men and women 70–89 years of age. The association between dietary protein intake and risk of hip fracture may be modified by age. Our study supports the hypothesis that adequate dietary protein is important for optimal bone health in the elderly 50–69 years of age
And against…
Protein Consumption and Bone Fractures in Women
Dietary protein increases urinary calcium losses and has been associated with higher rates of hip fracture in cross-cultural studies. However, the relation between protein and risk of osteoporotic bone fractures among individuals has not been examined in detail. In this prospective study, usual dietary intake was measured in 1980 in a cohort of 85,900 women, aged 35–59 years, who were participants in the Nurses’ Health Study. A mailed food frequency questionnaire was used and incident hip (n = 234) and distal forearm (n = 1,628) fractures were identified by self-report during the following 12 years. Information on other factors related to osteoporosis, including obesity, use of postmenopausal estrogen, smoking, and physical activity, was collected on biennial questionnaires. Dietary measures were updated in 1984 and 1986. Protein was associated with an increased risk of forearm fracture (relative risk (RR) = 1.22, 95% confidence interval (Cl) 1.04–1.43, p for trend = 0.01) for women who consumed more than 95 g per day compared with those who consumed less than 68 g per day. A similar increase in risk was observed for animal protein, but no association was found for consumption of vegetable protein. Women who consumed five or more servings of red meat per week also had a significantly increased risk of forearm fracture (RR = 1.23, 95% Cl 1.01–1.50) compared with women who ate red meat less than once per week. Recall of teenage diet did not reveal any increased risk of forearm fracture for women with higher consumption of animal protein or red meat during this earlier period of life. No association was observed between adult protein intake and the incidence of hip fractures, though power to assess this association was low.
The association between dietary protein intake and bone mass accretion in pubertal girls with low calcium intakes.
To assess the association between protein intakes and bone mass accrual in girls, data were analysed for 757 pre-pubertal girls (mean age 10.1 years) in urban Beijing, China, who participated in a 5-year study including 2 years of milk supplementation (intervention groups only) and 3 years of follow-up study. At 0, 12, 24, 48 and 60 months from the baseline, bone mass of the proximal or distal forearm (PF or DF) and total body (TB) was measured with dual energy X-ray absorptiometry; dietary intakes were assessed by a 3-d food record (including two weekdays and one weekend day). Linear mixed models were used and continuous variables were logarithm transformed. The mean longitudinal Ca intake (432-675 mg/d on average) positively influenced bone mineral content (BMC) at TB, PF and DF after controlling for baseline bone mass and other possible confounders. However, negative associations were observed between protein intake (55.9-61.0 g/d on average) and BMC accrual at TB, PF or DF (beta = – 1.92, – 10.2 or – 4.82, respectively, P < 0.01) after adjustment. When protein intake was considered according to animal or plant food sources, protein from animal foods, particularly meat, had significant negative effects on BMC accrual at DF or PF after adjustment. It was concluded that higher protein intake, especially from animal foods, appeared to have a negative effect on bone mass accrual in Chinese pubertal girls with low Ca intakes.
A high ratio of dietary animal to vegetable protein increases the rate of bone loss and the risk of fracture in postmenopausal women. Study of Osteoporotic Fractures Research Group.
RESULTS: Bone mineral density was not significantly associated with the ratio of animal to vegetable protein intake. Women with a high ratio had a higher rate of bone loss at the femoral neck than did those with a low ratio (P = 0.02) and a greater risk of hip fracture (relative risk = 3.7, P = 0.04). These associations were unaffected by adjustment for age, weight, estrogen use, tobacco use, exercise, total calcium intake, and total protein intake. CONCLUSIONS: Elderly women with a high dietary ratio of animal to vegetable protein intake have more rapid femoral neck bone loss and a greater risk of hip fracture than do those with a low ratio. This suggests that an increase in vegetable protein intake and a decrease in animal protein intake may decrease bone loss and the risk of hip fracture. This possibility should be confirmed in other prospective studies and tested in a randomized trial.
Protein Intake, Weight Loss, and Bone Mineral Density in Postmenopausal Women
Background. Higher protein diets are promoted for effective weight loss. Striated tissues in omnivorous diets contain high-quality protein, but limited data exist regarding their effects on bone. Methods. To examine the effects of energy restriction–induced weight loss with higher protein omnivorous diets versus lower protein vegetarian diets on bone mineral density in overweight postmenopausal women, two randomized controlled feeding studies were conducted. In Study 1, 28 women consumed 750 kcal/day energy deficit diets with 18% energy from protein via lacto-ovo vegetarian sources (normal protein, n = 15) or 30% energy from protein with 40% of protein from lean pork (higher protein, n = 13, omnivorous) for 12 weeks. In Study 2, 54 women consumed their habitual diet (control, n = 11) or 1,250 kcal/day diets with 16% energy from nonmeat protein sources (n = 14) or 26% energy from protein, including chicken (n = 15) or beef (n = 14) for 9 weeks.Results. Study 1: With weight loss (normal protein −11.2%, higher protein −10.1%), bone mineral density was not significantly changed in normal protein (−0.003 ± 0.003 g/cm2, −0.3%) but decreased in higher protein (−0.0167 ± 0.004 g/cm2, −1. 4%, group-by-time p < .05). Study 2: The control, nonmeat, chicken, and beef groups lost 1.5%, 7.7%, 10.4%, and 8.1% weight and 0.0%, 0.4%, 1.1%, and 1.4% bone mineral density, respectively. The change of bone mineral density was significant for chicken and beef compared with the control (group-by-time, p < .05). Markers of calcium metabolism and bone homeostasis in blood and urine were not changed over time or differentially affected by diet.
It has to be observed that the last one is studying the efects of pretty low calorie diets, and is therefore not extractable to a normal lifestyle. Weight loss is associated with losing bone mass in other studies 1, and it’s fair top assume that on a intake that low other dietary factors necessary for bone strength might have been lacking. I’d also like to comment that the 95g of animal protein needed to negatively bone mass in one of the others is more than the American national average of 91g, 2, and seems to mostly limited to heavy consumers of red meat. So, also not a damning indictment of the average level of animal proteins in the western diet. I’d also like to add that the Chinese are largely lactose intolerant and don’t have a history of dairy consumption, and a negative effect of dairy on the lactose intolerant’s bone mass has been observed in at least one other study, so, again, other factors may be affecting the outcome of the Chinese study.
I’m noticing a trend for fish to be excluded from the studies that cause bone loss as a cause, with some evidence that fish, particluarly the omega three oils, are beneficial to bone mass.
And to finish all of this, the meta studies (overviews and combination of all other available studies)…
Dietary protein and bone health: a systematic review and meta-analysis.
BACKGROUND: There has been a resurgence of interest in the controversial relation between dietary protein and bone health. OBJECTIVE: This article reports on the first systematic review and meta-analysis of the relation between protein and bone health in healthy human adults. DESIGN: The MEDLINE (January 1966 to September 2007) and EMBASE (1974 to July 2008) databases were electronically searched for all relevant studies of healthy adults; studies of calcium excretion or calcium balance were excluded. RESULTS: In cross-sectional surveys, all pooled r values for the relation between protein intake and bone mineral density (BMD) or bone mineral content at the main clinically relevant sites were significant and positive; protein intake explained 1-2% of BMD. A meta-analysis of randomized placebo-controlled trials indicated a significant positive influence of all protein supplementation on lumbar spine BMD but showed no association with relative risk of hip fractures. No significant effects were identified for soy protein or milk basic protein on lumbar spine BMD. CONCLUSIONS: A small positive effect of protein supplementation on lumbar spine BMD in randomized placebo-controlled trials supports the positive association between protein intake and bone health found in cross-sectional surveys. However, these results were not supported by cohort study findings for hip fracture risk. Any effects found were small and had 95% CIs that were close to zero. Therefore, there is a small benefit of protein on bone health, but the benefit may not necessarily translate into reduced fracture risk in the long term.
So, no evidence of bone loss from protein here…
Protein intake and bone health: a systematic review and meta-analysis
These effects suggest that dietary protein may have a beneficial effect on BMD.
And no loss of bone mass here either. Essentially, when considering all the studies, there is no evidence of loss, but some of slight gain.
Other, relevant info…
Supplementing rats diets with fish peptides improved their bone density
Fish oil improves BMD in mice
Fish improves bone density in Astronauts,
Dietary protein supplementation increases peak bone mass acquisition in energy-restricted growing rats.
Ratio of potassium to protein affects bone loss
Potassium, magnesium, and fruit and vegetable intakes are associated with greater bone mineral density in elderly men and women
Potassium Citrate Boosts Bone Density in the Elderly
The effects of high potassium consumption on bone mineral density in a prospective cohort study of elderly postmenopausal women.
Magnesium improves bone density.
So, from spending a couple of days searching through the studies, I can tell you that animal protein in the diet has most likely a slight positive effect, there’s nothing that suggests fish has anything but a positive effect, and that if any animal protein has a poor effect it is going to be red meat, and only if you eat a lot of it. I also tracked down three meta studies of dairy consumption (combined studies of all the previous studies) and the overwhelming conclusion was that diary has a slight to zero improvement on bone mass, not at all a loss, as is so often claimed.
Anyone concerned about their bone mass should… eat a healthy variety and amount of protein ( flesh, dairy or otherwise, but some fish in there is probably healthiest) and plenty of fruit and veg and nuts (for the potassium, calcium and magnesium). They should also get plenty of load bearing exercise, but avoid alcohol, smoking and phosphoric acid laden soda drinks and salt (which are all associted with mineral loss). The overall healthier diets and lifestyle of vegetarians is the reason they have better health (excepting pescatarians), not the lack of flesh.
I’d like to add, the human diet for most of out evolutuionary existance has been over 2/3 animal flesh calories; paleolithic bones and the bones of contemporary hunter gatherers who eat mainly a flesh based diet are robust as hell. They need to be as hunters have to survive extremely violent impacts quite frequently when subduing their prey. The whole concept that the diet we evolved to eat makes us frail boned is against all logic.